The June cover of Critical Care Nurse features an article on Routine Neurological Assessments by Nurses in the Pediatric Intensive Care Unit (Kirschen et al., 2019) which discusses a quality improvement intervention over a 1-year period. The goal was to standardize neurological assessments by nursing staff, improve the compliance of providers entering orders, improve nursing documentation, and assess the frequency of neurological decline before admission and after discharge. The study successfully improved ordering and documenting neurological assessments and found that patients with developmental disabilities were more likely to experience a decline in neurological status than patients who do not have a developmental disability.
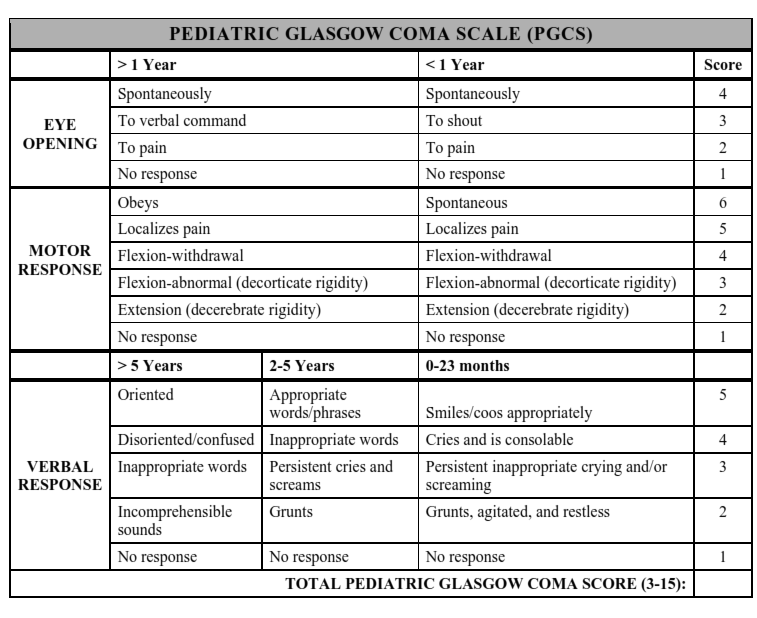
How is this relevant to the pediatric CCRN exam? Clinical inquiry includes questioning the appropriateness of policies, guidelines, and current practices to continuously improve patient outcomes. Identifying and addressing differences in practice are important in clinical inquiry to ensure that best practices are followed. Standardization in ordering and documenting neurological assessments is important in identifying objective patient declines in order to intervene early and appropriately. While blood pressure, heart rate, and intracranial pressure are objective measures of neurological assessment, the use of the Glasgow Coma Scale may vary from nurse to nurse.
Clinical inquiry is a Professional Caring and Ethical Practice in the American Association of Critical Care Nurses (AACN) synergy model, which defines patient characteristics and nurse characteristics explaining how they can best be combined to improve outcomes. Professional Caring and Ethical Practice encompasses 20% (80 questions) of the pediatric CCRN exam.
Kirschen, M. P., Lourie, K., Snyder, M., Agarwal, K., DiDonato, P., Kraus, B., ...Topjian, A. (2019). Routine Neurological Assessments by Nurses in the Pediatric Intensive Care Unit. Critical Care Nurse, 39(3), 20-32.
Photo credit: http://boneandspine.com/wp-content/uploads/2013/08/pediatric-glsagow-coma-scale.png